| Total CBD: | 500 – 2500 mg |
| Potency: | 16.6 - 83.3 mg/mL |
| Cost per mg CBD: | $0.12 – $0.18 |
| Extract Type: | Full-spectrum |
| THC Content: | <0.3% |

Evidence based
CBD For Diabetes: Benefits, Dosage, & Side-Effects
Studies have shown that those taking cannabis on a regular basis are less likely to develop diabetes.
How does this work? Can CBD oil help manage or prevent diabetes?
Roughly 1 in every 3 people have diabetes or pre-diabetes in the United States today.
One of the most promising solutions put forward in recent years is CBD.
A study done in 2013 noticed a correlation between regular cannabis use and a lower incidence of metabolic syndrome, obesity, and diabetes – despite the users generally having poorer diets than average [4].
Here, we investigate the causes of diabetes, and how CBD can be used to improve the quality of life of someone suffering from this medical condition.
The Best CBD Oils for Diabetes
- Royal CBD Oil — Best CBD Oil Overall
- Gold Bee CBD Oil — Best Organic CBD Oil
- Endoca CBD Oil — Best CBD Oil For Diabetes (Europe)
What Are The Benefits of CBD Oil For Diabetes?
We’ll delve deep into this complex and fascinating topic, before we dive in, here are the main benefits of CBD for diabetes:
- Promotes weight loss by reducing appetite [13]
- Alleviates side-effects of diabetes (such as neuropathic pain)
- Protects the liver
- May reduce insulin resistance [4]
- Speeds wound healing [10]
- Protects the insulin-secreting cells in the pancreas [5]
CBD oil has many benefits regarding diabetes, and there are even a few pharmaceuticals in the pipeline that use synthetic cannabinoids as an active ingredient.
This is a large and complex topic, but we aim to break it down into easily digestible chunks. We’ll help you understand how CBD oil may be able to improve diabetes symptoms, and why this and other potentially useful cannabinoids should be on the radar for anybody looking to do that.
Related: Best CBD:THC Ratio for Neuropathic Pain.
1. May Promote Weight Loss
Obesity is considered one of the main contributing factors for the development of diabetes [2].
CBD offers direct benefits to fight obesity. It reduces the desire to eat through the reward system in the brain (responsible for habits and addiction), as well as through the endocannabinoid CB1 receptors.
These receptors are found primarily in the brain and central nervous system and regulate the hormones associated with hunger [3].
With less hunger, in theory, we eat less food. By helping us eat less, especially refined or overly processed foods, we may be able to start reducing weight and slowing the progression of diabetes.
2. Alleviates Common Side-Effects of Diabetes
On top of all the potential benefits CBD oil may offer to the processes driving diabetes, it also offers some unique benefits towards treating the symptoms of the condition. Of course, further research is needed in all these areas to confirm and better standardize how CBD might be used effectively.
Some examples of symptoms CBD addresses include:
- Lowers nerve pain [8,12]
- Reduces anxiety [9]
- Speeds healing (topically) [10]
- Curbs appetite for sweet foods [11]
3. Supports Insulin Production & Pancreas Health
A recent study involving nearly 4700 patients with diabetes or prediabetes were screened to measure marijuana use and insulin sensitivity. Researchers in this study concluded that “marijuana use was associated with lower levels of fasting insulin” [4].
The study found that marijuana users had a 16% decrease in insulin resistance.
This suggests that cannabis makes insulin more effective at doing its job, which is the main cause of diabetes. With insulin working the way it should, we’re better able to manage our blood sugar levels.
This slows the onset of diabetes and prolongs lifespan.
Looking closely, researchers discovered that, in animal trials, overweight or obese rats given cannabis over long periods of time had a heavier pancreas [5].
This suggests that cannabis was able to protect the insulin-secreting pancreatic beta cells from damage caused by obesity.
This is very important when we consider the fact that the main problem with diabetes is damage to the pancreas, which eventually leads to the development of the more severe, type-1 diabetes. Unfortunately, by the time type 1 diabetes is diagnosed, the patient may have already lost up to 50% of their insulin secretory capability.
What is Diabetes? Signs, Symptoms, Risks
Before getting into the nitty-gritty about how CBD could help with diabetes, it helps to understand some of the important details about how diabetes works.
Diabetes is a metabolic condition. It’s a disease involving our ability to process carbohydrates in the body.
Most of our energy comes from sugar.
Whenever we eat something, sugars from the foods enter the bloodstream through the digestive tract.
The cells then need to use this sugar to power activity. Unfortunately, sugar can’t get into the cell without a special escort, known as insulin.
Insulin is a hormone released by the pancreas, responsible for regulating how much sugar moves from the blood into the cells.
When we have diabetes, we either don’t have enough insulin to do the job (type-1 diabetes), or the insulin we do have is being ignored by the body (type-2 diabetes). With both types, the results are almost the same — an increased blood sugar profile.
Our cells begin to starve for energy, while the blood becomes thick with sugar.
This causes all kinds of problems for the body, especially on the liver, skin, kidneys, and cardiovascular system.
In essence, diabetes is a very serious disease involving the dysfunctional production of insulin by the pancreas.
There are two main types of diabetes:
Type-1 Diabetes
This form of diabetes is often referred to as juvenile-onset diabetes because it usually starts showing up during childhood or adolescence.
It involves dysfunctional pancreatic beta cells, which are responsible for producing insulin.
This type of diabetes will require sufferers to inject themselves with insulin for the rest of their lives because their body can’t produce enough for itself. If they don’t have access to insulin, the imbalance of insulin: glucagon will cause the liver to make too much glucose and ketone acids resulting in a metabolic emergency called Diabetic Ketoacidosis.
CBD only offers mild support for these patients — not emergency support.
Type-2 Diabetes
Type 2 diabetes is often referred to as adult-onset diabetes because the people affected usually manifest it after the age of 40 — however, recently there is greater incidence in younger populations.
Though there might be a genetic predisposition to it, the actual development of the disease is slow and gradual, caused mainly by poor diet and lifestyle choices.
Whenever we eat a meal, our digestive system slowly breaks the food down. The resulting nutrients – sugars, proteins, fat, etc. – will be absorbed into the bloodstream.
This makes us feel energized directly after the meal because we suddenly have a ton of energy available.
The pancreas then rushes to secrete insulin to move the sugar from the blood to the cells. It does this because we always want to maintain a steady blood sugar level: too much is bad, and too little is bad.
Unfortunately, if the food we ate was high in simple sugars (like candy or white bread), it gets digested very fast, and insulin will quickly remove most of the sugar in the blood. Too much in fact. Without blood sugar, we feel fatigued and low in energy.
We often refer to this as a crash after a meal — especially a high-carb one.
It’s the reason why many people feel dull and low in energy about an hour or two after lunch.
Over many years, these sudden spikes and crashes in blood glucose levels will train the body to ignore the insulin. It does this in an attempt to maintain blood sugar levels stable.
We call this stage insulin resistance. It’s the first step towards type-2 diabetes.
Now we have a problem.
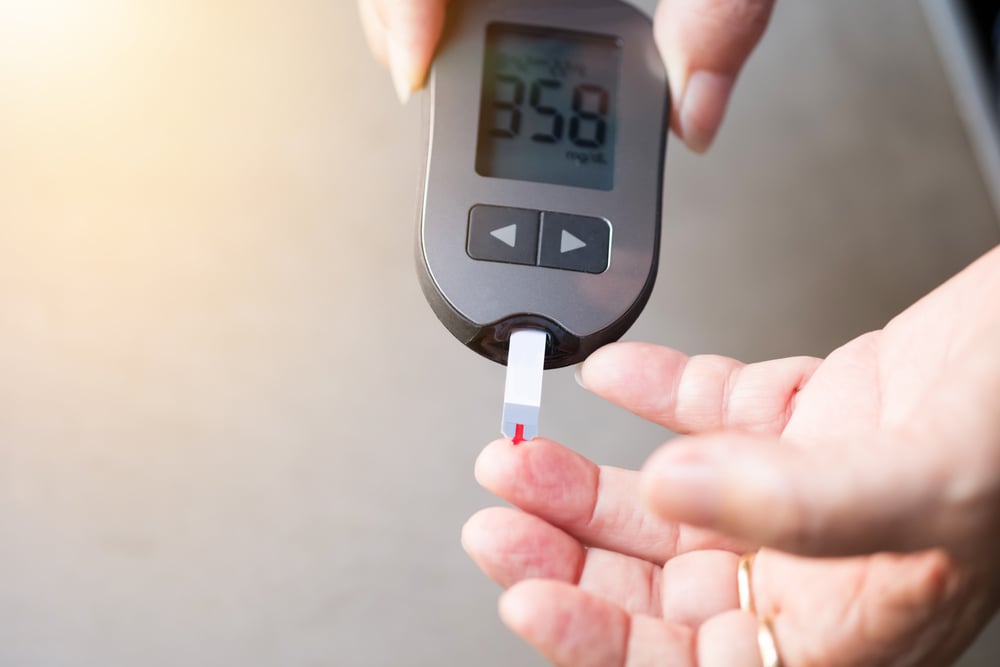
Sugar levels rise in the blood but decrease inside the cells themselves; after all, insulin is not working properly. The cells then send signals to the brain to eat more food, causing sugar cravings. But no matter how much we eat, we can’t seem to give our cells what they want.
High blood sugar is dangerous. It can damage our red blood cells, blood vessel linings, kidneys, and lungs.
If blood sugar spikes too high, too quickly, then a potentially dangerous, dehydrating condition called hyperglycemic hyperosmolar nonketotic syndrome can develop. The body needs to do something else to keep blood sugar levels in check.
So it turns to the liver.
The liver is now tasked with converting all this excess sugar into something safer, such as fat, leading to increased weight gain and fat deposits in the liver (fatty liver disease).
This is the reason for the characteristic “belly fat” many diabetics have. It’s caused by fat deposits forming around the liver and other organs in the abdomen.
Over time, if left unchecked, type-2 diabetes will gradually worsen, and blood sugar levels will rise to the point where they start to cause damage to the kidneys, lungs, cardiovascular system, and pancreas.
People with diabetes stand 2-4 times the risk of cardiovascular disease and have a life expectancy of 5-10 years less than non-diabetics. It’s the number one cause of kidney failure, non-traumatic amputations, and blindness in the developed world — and it is the 7th leading cause of death in the U.S. Fortunately, diabetes is very treatable through improved lifestyle changes and medication.
In fact, late-stage type 2 diabetics will eventually develop type 1 diabetes due to damage to the pancreas. This is why people with late-stage type-2 diabetes need to take insulin shots like a person with type-1 diabetes.
CBD offers some potent benefits for reducing the impact of type 2 diabetes and is becoming an important therapeutic option for people suffering from this condition.
What Causes Diabetes?
So, now that we’ve learned how diabetes works and what the different kinds are, let’s discuss what actually causes it.
Type-1 diabetes is mainly a genetic condition, but can also be caused by toxic exposure. Some compounds, such as streptozotocin are well-known to kill the beta-cells in the pancreas, causing type-1 diabetes. This compound is used to induce diabetes in mice for research purposes.
Other compounds such as second-hand smoke and hydrocarbons from car exhausts have also been linked to type-1 diabetes[1]; however, the majority of cases are caused by genetic factors.
Type-2 diabetes is primarily caused by diets that are high in refined carbohydrates (simple sugars), but low in fiber, fat, and antioxidants.
The repeated spikes and crashes in blood sugar levels are the ones that eventually lead to insulin resistance, with an increase in cravings which damages metabolic balance in the body even further. This paves the path towards diabetes.
How is Diabetes Treated?
There is no cure for either type-1 or type-2 diabetes. However, many experts argue type-2 may be reversed over time with significant lifestyle and diet changes.
Most modern treatments look at resolving the symptoms, preventing further complications, and holding what we would call hyperglycemia (high blood sugar) at bay by promoting the production or sensitivity of insulin, in order to prevent worsening of the disease and further damage. Type-1 patients will also use insulin to keep their insulin: glucagon ratio in balance to manage ketone acids and blood sugars.
Because high blood sugar causes most of the damage in the disease, monitoring blood sugar levels, proper nutrition, and exercise will all contribute to improving the negative effects of the condition.
Conventional Treatments for Diabetes May Include:
- Mediterranean diet (the most evidence-supported diet)
- Metformin (improves sensitivity to insulin)
- Sulfonylureas (promote the release of more insulin)
- Meglitinides (promote the release of more insulin)
- Thiazolidinediones (improve sensitivity to insulin)
- DPP-4 inhibitors (modestly increase insulin levels)
- GLP-1 receptor agonists (slow the rate of sugar absorption in the gut)
- SGLT2 inhibitors (stop the kidneys from reabsorbing filtered sugar)
- Insulin (provides insulin to type 1 and late-stage type 2 diabetics)

Other Treatments
Since diabetes is a condition that involves a problem with the balance of our metabolic system, CBD may offer some potentially serious therapeutic benefits to the actual cause of the condition.
Some examples include:
- Atkins diet (high fat and protein, low carbohydrates)
- Modified Atkins diet (similar to Atkins but more focus on high-fat meals)
- Ketogenic diet (low carb, medium protein, high fat)
- Chromium supplementation
- Regular exercise
- Herbal supplements (cinnamon, ginseng, gymnema, gynostemma)
- Acupuncture
- Lifestyle changes (quitting smoking and alcohol)
All these treatment options are good, and there’s no one treatment for the condition that’s better than the rest. The best treatment plan will use a combination of the above options.
Recent evidence has suggested another potential treatment option through CBD.
The use of this compound for diabetes offers some unique benefits to the condition and may go a long way in enhancing the effectiveness of these other treatment options.
How to Use CBD Oil for Diabetes
Now that we understand how CBD oil might support people with diabetes, and how promising the advancement of further research could be, let’s talk about how people are using it.
1. Adding CBD to Other Interventions
For starters, it’s important to remember that CBD oil is best used in addition to other interventions, especially the ones revolving around changes in diet and lifestyle.
Anybody with diabetes should make a focused effort toward avoiding refined carbohydrates and increasing the consumption of fats and proteins.
On top of this, mild to moderate exercise and stress management techniques will go a long way in addressing the causes of diabetes and slowing its progression.
It’s also important to note that you should never stop taking any medication without first consulting with your doctor. Always take medications as directed, and keep regular track of your blood sugars.
Diabetes is a complicated problem and there are a lot of factors that need to be considered. A trained medical professional is going to be the best person to speak with regarding your treatment options.
2. Recommended Dosage of CBD for Diabetes
The right dose of CBD oil is different for everybody.
The endocannabinoid system works through is different from one person to the next.
This can make figuring out the proper dose a difficult process.
Generally speaking, the dose most commonly used for diabetics is between 2.5 mg and 100 mg of CBD per day.
This is a large range, so the best way to do it is to start small and build up slowly until you start to get the desired effects.
Most people will start with 1 or 2 mg equivalents and add 4 mg per day.
If side effects are noticed (such as fatigue, poor focus or concentration, or headaches) then simply reduce the dose to the last one that didn’t produce side effects. And stay there.
When managing diabetes with your prescriptions, integrated with taking CBD oil, it’s important to first speak with your doctor. In most cases, the long-term use of CBD is required for the potential changes listed above.
References
- Bodin, J., Stene, L. C., & Nygaard, U. C. (2015). Can exposure to environmental chemicals increase the risk of diabetes type 1 development?. BioMed Research International, 2015.
- Grundy, S. M., Cleeman, J. I., Merz, C. N. B., Brewer, H. B., Clark, L. T., Hunninghake, D. B., … & Coordinating Committee of the National Cholesterol Education Program. (2004). Implications of recent clinical trials for the national cholesterol education program adult treatment panel III guidelines. Journal of the American College of Cardiology, 44(3), 720-732.
- Matias, I., & Di Marzo, V. (2006). Endocannabinoid synthesis and degradation, and their regulation in the framework of energy balance. Journal of endocrinological investigation, 29(3), 15.
- Penner, E. A., Buettner, H., & Mittleman, M. A. (2013). The impact of marijuana use on glucose, insulin, and insulin resistance among US adults. The American journal of medicine, 126(7), 583-589.
- Levendal, R. A., Schumann, D., Donath, M., & Frost, C. L. (2012). Cannabis exposure associated with weight reduction and β-cell protection in an obese rat model. Phytomedicine, 19(7), 575-582.
- Migrenne, S., Lacombe, A., Lefevre, A. L., Pruniaux, M. P., Guillot, E., Galzin, A. M., & Magnan, C. (2009). Adiponectin is required to mediate rimonabant-induced improvement of insulin sensitivity but not body weight loss in diet-induced obese mice. American Journal of Physiology-Regulatory, Integrative and Comparative Physiology, 296(4), R929-R935.
- Purohit, V., Rapaka, R., & Shurtleff, D. (2010). Role of cannabinoids in the development of fatty liver (steatosis). The AAPS journal, 12(2), 233-237.
- Serpell, M., Ratcliffe, S., Hovorka, J., Schofield, M., Taylor, L., Lauder, H., & Ehler, E. (2014). A double‐blind, randomized, placebo‐controlled, parallel group study of THC/CBD spray in peripheral neuropathic pain treatment. European journal of pain, 18(7), 999-1012.
- Crippa, J. A. S., Derenusson, G. N., Ferrari, T. B., Wichert-Ana, L., Duran, F. L., Martin-Santos, R., … & Filho, A. S. (2011). Neural basis of anxiolytic effects of cannabidiol (CBD) in generalized social anxiety disorder: a preliminary report. Journal of Psychopharmacology, 25(1), 121-130.
- Wright, K., Rooney, N., Feeney, M., Tate, J., Robertson, D., Welham, M., & Ward, S. (2005). Differential expression of cannabinoid receptors in the human colon: cannabinoids promote epithelial wound healing. Gastroenterology, 129(2), 437-453.
- Morgan, C. J., Freeman, T. P., Schafer, G. L., & Curran, H. V. (2010). Cannabidiol attenuates the appetitive effects of Δ 9-tetrahydrocannabinol in humans smoking their chosen cannabis. Neuropsychopharmacology, 35(9), 1879.
- Deshpande, A., Mailis-Gagnon, A., Zoheiry, N., & Lakha, S. F. (2015). Efficacy and adverse effects of medical marijuana for chronic noncancer pain: Systematic review of randomized controlled trials. Canadian Family Physician, 61(8), e372-e381.
More Health Conditions to Explore
-
Conditions Related to Health Benefits
- CBD For Allergies: Can This Cannabinoid Ease Symptoms?
- Top 10 CBD Oils For Back Pain
- Can CBD Help With Menstrual Cramps?
- CBD for Sciatica: How It Works, Safety, Drug Interactions, & Best Products
- Is CBD a Viable Treatment for Cerebral Palsy?
- CBD Oil For Sleep
- CBD For Psoriasis: Can CBD Help to Alleviate Symptoms?
- Traumatic Brain Injury (TBI)
- Arthritis
- Anxiety & Depression
- Weight Loss
- ADD & ADHD
- Anorexia
- Alzheimer’s Disease & Dementia
- Addiction
- ALS (Amyotrophic Lateral Sclerosis)
- Antibiotic Resistance
- Asthma
- Atherosclerosis
- Autism
- Acne
- Bipolar Disorder
- Pain
- Crohn's Disease & Ulcerative Colitis
- Diabetes
- Epilepsy
- Endocrine Disorders
- Fibromyalgia
- Fatty Liver Disease
- Glaucoma
- Hypertension
- Heart Disease
- Huntington's Disease
- Inflammation
- Irritable Bowel Syndrome (IBS)
- Kidney Disease
- Migraine Headaches
- Muscle Recovery
- Multiple Sclerosis
- Motion Sickness
- Metabolic Syndrome
- Neurodegeneration
- Cancer
- Nausea
- Neuropathic (Nerve) Pain
- Osteoporosis/Bone Health
- Obsessive-Compulsive Disorder (OCD)
- Polycystic Ovarian Syndrome (PCOS)
- PTSD
- Prion/Mad Cow Disease
- Premenstrual Syndrome (PMS)
- Parkinson’s Disease
- Schizophrenia
- Sickle Cell Anemia
- Stroke
-
Conditions Related to Products
- Ranking The Top 13 THC Gummies By Category (Δ8, Δ9, Δ10, HHC, & More)
- Top 10 CBD Oils For Back Pain
- Everything You Need to Know About CBD Sunscreen
- Top 7 CBD Gummies For Sleep & Insomnia
- Top 7 CBD Gummies To Help With Anxiety (2022)
- Best CBD Gummies For Pain (Top-Rated Pain Gummies For 2022)
- Best Hemp Cigarettes (Top 5 Nicotine-Free Smokes)
- Top 5 CBD Lip Balms For 2022
- The Top 7 CBD Face Masks for 2022
- The Best CBD Inhalers For 2022 (& How to Use Them)
- Best Full-Spectrum CBD Vape Juice: What to Look For & How to Use It
- CBD Eye Drops: New Option For Glaucoma?
- CBD Oil For Dogs With Arthritis
- Best CBD Massage Oils In 2022
- Buyer's Guide To The Best CBD Vape Kits In 2022
- CBD Chocolate: Yes, It Exists & It's Just as Divine as it Sounds
- CBD Pre-Rolls & Cigarettes
- Terpene Concentrates
- Best CBD Soaps
- Best CBD Shampoo & Conditioner
- Best CBD Juul Pods
- CBD Isolate Oils
- Full-Spectrum CBD Oils
- Best CBD Lube
- CBD Honey
- CBD Transdermal Patches
- Best Dry Herb Vaporizers
- CBD Oil For Dogs With Epilepsy
- CBD Oil For Dogs With Anxiety
- CBD Oil For Dogs With Cancer
- CBD For Horses
- CBD Chewing Gum
- CBD Pain Cream
- CBD Oil For Cats
- CBD Oil For Dogs
- CBD Hemp Flower
- CBD Suppositories
- Best CBD Gummies for Pain, Sleep & Anxiety Reviewed (2022)
- CBD Teas
- CBD Vape Pens
- CBD Vape Oils
- CBD Coffee
- CBD Drinks & Shots
- CBD Crystals
- CBD Skincare
- Best CBD Oil & Gummies For Kids: Is CBD Safe for Children with Anxiety & ADHD?
- CBD Concentrates
- CBD Bath Bombs
- CBD Capsules
- CBD Sprays
- CBD Dog Treats
-
Conditions Related to Topicals
-
Conditions Related to Oils & Tinctures
-
Conditions Related to Edibles
- Top 7 CBD Gummies To Help With Anxiety (2022)
- Best CBD Gummies For Pain (Top-Rated Pain Gummies For 2022)
- CBD Chocolate: Yes, It Exists & It's Just as Divine as it Sounds
- CBD Honey
- CBD Chewing Gum
- Best CBD Gummies for Pain, Sleep & Anxiety Reviewed (2022)
- CBD Teas
- CBD Coffee
- CBD Drinks & Shots
- CBD Capsules
-
Conditions Related to Gummies
- Ranking The Top 13 THC Gummies By Category (Δ8, Δ9, Δ10, HHC, & More)
- Top 7 CBD Gummies For Sleep & Insomnia
- Top 7 CBD Gummies To Help With Anxiety (2022)
- Best CBD Gummies For Pain (Top-Rated Pain Gummies For 2022)
- Best CBD Gummies for Pain, Sleep & Anxiety Reviewed (2022)
- Best CBD Oil & Gummies For Kids: Is CBD Safe for Children with Anxiety & ADHD?
-
Conditions Related to Hemp Flower
-
-
Conditions Related to Terpenes
-
-
Conditions Related to Cultivation
-
Conditions Related to Concentrates
-
Conditions Related to Delta 8 THC
-
Conditions Related to Delta 9 THC
-
-
-
-
Conditions Related to CBD
- Everything You Need to Know About CBD Sunscreen
- Top 7 CBD Gummies For Sleep & Insomnia
- Top 7 CBD Gummies To Help With Anxiety (2022)
- Best CBD Gummies For Pain (Top-Rated Pain Gummies For 2022)
- Best Hemp Cigarettes (Top 5 Nicotine-Free Smokes)
- Top 5 CBD Lip Balms For 2022
- The Top 7 CBD Face Masks for 2022
- The Best CBD Inhalers For 2022 (& How to Use Them)
- Best Full-Spectrum CBD Vape Juice: What to Look For & How to Use It
- CBD Eye Drops: New Option For Glaucoma?
- CBD Oil For Dogs With Arthritis
- Best CBD Massage Oils In 2022
- Buyer's Guide To The Best CBD Vape Kits In 2022
- CBD Chocolate: Yes, It Exists & It's Just as Divine as it Sounds
- CBD Pre-Rolls & Cigarettes
- Best CBD Soaps
- Best CBD Shampoo & Conditioner
- Best CBD Juul Pods
- CBD Isolate Oils
- Full-Spectrum CBD Oils
- Best CBD Lube
- CBD Honey
- CBD Transdermal Patches
- CBD Oil For Dogs With Epilepsy
- CBD Oil For Dogs With Anxiety
- CBD Oil For Dogs With Cancer
- CBD For Horses
- CBD Chewing Gum
- CBD Pain Cream
- CBD Oil For Cats
- CBD Oil For Dogs
- CBD Hemp Flower
- CBD Suppositories
- Best CBD Gummies for Pain, Sleep & Anxiety Reviewed (2022)
- CBD Teas
- CBD Vape Pens
- CBD Vape Oils
- CBD Coffee
- CBD Drinks & Shots
- CBD Crystals
- CBD Skincare
- Best CBD Oil & Gummies For Kids: Is CBD Safe for Children with Anxiety & ADHD?
- CBD Concentrates
- CBD Bath Bombs
- CBD Capsules
- CBD Sprays
- CBD Dog Treats
-
-
Conditions Related to THC-O
-
-
Conditions Related to Joint Health
-
Conditions Related to Pain Disorders
- Top 10 CBD Oils For Back Pain
- Can CBD Help With Menstrual Cramps?
- CBD for Sciatica: How It Works, Safety, Drug Interactions, & Best Products
- Traumatic Brain Injury (TBI)
- Arthritis
- Pain
- Fibromyalgia
- Glaucoma
- Inflammation
- Kidney Disease
- Migraine Headaches
- Multiple Sclerosis
- Neuropathic (Nerve) Pain
- Premenstrual Syndrome (PMS)
- Sickle Cell Anemia
-
Conditions Related to Autoimmune Disease
-
Conditions Related to Cognitive Health
-
Conditions Related to Metabolic Disorders
-
Conditions Related to Psychological Disorders
-
Conditions Related to Muscles & Bones
-
Conditions Related to Nervous System
- CBD for Sciatica: How It Works, Safety, Drug Interactions, & Best Products
- Is CBD a Viable Treatment for Cerebral Palsy?
- CBD Oil For Sleep
- Traumatic Brain Injury (TBI)
- Anxiety & Depression
- ADD & ADHD
- Anorexia
- Alzheimer’s Disease & Dementia
- Addiction
- ALS (Amyotrophic Lateral Sclerosis)
- Autism
- Bipolar Disorder
- Epilepsy
- Huntington's Disease
- Inflammation
- Migraine Headaches
- Multiple Sclerosis
- Motion Sickness
- Neurodegeneration
- Neuropathic (Nerve) Pain
- Obsessive-Compulsive Disorder (OCD)
- PTSD
- Prion/Mad Cow Disease
- Parkinson’s Disease
- Schizophrenia
-
-
Conditions Related to Reproductive Health
-
Conditions Related to Hormones & Endocrine
-
Conditions Related to Skin Health
-
Conditions Related to Cardiovascular System
-
Conditions Related to Digestive System
-
Conditions Related to Genetic Disorders
-
Conditions Related to For Children